 Healthcare consolidation is on a tear, with several massive deals at the end of 2017, including CVS-Aetna and UnitedHealth Group buying one of the largest U.S. physician groups. Hospitals are merging in ever-larger deals, creating multi-state powerhouses. The number of U.S. hospitals that are part of a system rose nearly 20% between 2006 and 2016, according to the American Hospital Association (AHA).
Healthcare consolidation is on a tear, with several massive deals at the end of 2017, including CVS-Aetna and UnitedHealth Group buying one of the largest U.S. physician groups. Hospitals are merging in ever-larger deals, creating multi-state powerhouses. The number of U.S. hospitals that are part of a system rose nearly 20% between 2006 and 2016, according to the American Hospital Association (AHA).
Healthcare companies also are forging creative alliances, with some of the industry’s biggest investments now happening outside the traditional hospital setting. Here are three trends to watch in 2018 and what they might mean for healthcare analytics.
Why consolidate?
Healthcare mergers, acquisitions, and other forms of partnerships are on a steady march for a few reasons as providers try to contain costs while delivering quality care. Many organizations are not equipped to navigate the rapidly changing industry and the move toward value-based care on their own, so they are looking for partners that complement and strengthen them. Other benefits include:
- Cost-savings through consolidating back office functions and supply chains
- Increased leverage in bargaining with payers and suppliers
- Increased capacity to collect and analyze data to improve efficiency and quality of care
Trend #1: Growth in outpatient settings
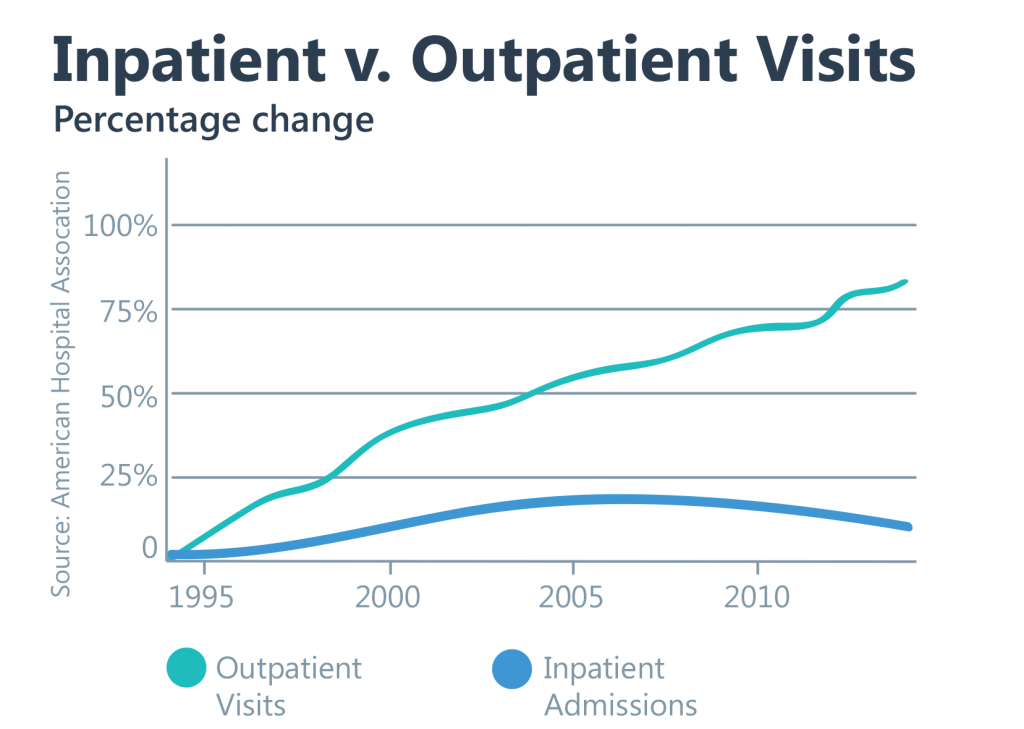
Healthcare consumers increasingly seek lower-cost and more convenient options for medical care, especially for minor complaints such as ear infections. AHA data shows that visits to outpatient facilities have soared recently while hospital demand has slowed. There also is strong growth in the number of surgeries performed outside of hospitals, where prices can be significantly lower.
To keep competitors from siphoning off their patients, hospitals are getting into the outpatient game, aggressively acquiring surgery centers, urgent care clinics, and free-standing emergency rooms. HCA, the largest publicly traded U.S. hospital company, has increased its number of urgent care centers 40% over two years and doubled its free-standing emergency rooms to 64. Sutter Health, Tenet Healthcare, and Advocate Health Care are investing heavily in outpatient clinics, while Tandem Hospital Partners is working with non-profit health systems to build 15-bed micro-hospitals. The hope is that patients who receive treatment in the smaller settings will choose the associated hospital when they need inpatient care.
Trend #2: Non-traditional partnerships
In addition to shifting services away from the expensive hospital setting, some healthcare companies are teaming up with non-traditional partners. These alliances offer significant opportunities in population health management.
For example, CVS Health’s proposal to buy Aetna made headlines last month not only because of its $69 billion price tag, but for the potential new ways to deliver healthcare. CVS already operates 1,100 walk-in clinics and owns Caremark, which manages pharmacy benefits for 75 million members. The combination of retail health, pharmacy, and payer services would bring together several streams of information. This could be used to reduce health care costs by:
- Better tracking patients between visits
- Tracking medication adherence through prescriptions filled and refilled
- Reducing delays in care that sometimes lead to more severe illnesses
All of this information could then be fed into population health management programs to better understand and support patients, especially those with chronic conditions, and keep a lid on costs. In announcing the acquisition, CVS claimed hospital readmissions could be cut in half if patients and clinicians had a complete view of their medications after discharge!
CVS follows UnitedHealth Group in putting many elements of the healthcare system under one roof. UnitedHealth, the nation’s largest health insurer, has purchased hundreds of medical clinics, urgent care and surgery centers in the past few years. It also owns Optum, a multi-faceted company comprised of physician groups, prescription benefits management for 65 million people and a line of business services including data analytics, consulting, and population health. It is a diversified model, all aimed at keeping patients out of the hospital and limiting loss on medical care.
Trend #3: Privacy concerns
In these mega-companies, patients may benefit from better coordinated medical and pharmacy services, but the consolidations do raise privacy concerns. In addition to tracking prescriptions, CVS knows when customers add a candy bar or soda to their purchase! Combined with Aetna’s claim information, this gives CVS much greater visibility into patient behaviors. Again, there is great potential in population health improvements, but how comfortable will consumers be with one company knowing so much about them? Among the other vexing questions: Who owns that information and how will it be safeguarded?
Bottom line
All this healthcare consolidation reminds us just how dynamic the industry is now and how organizations are seeking acquisitions and alliances to hedge against uncertainties. Many different types of healthcare organizations share the same goal: good patient outcomes without unreasonable spending. Where all this goes remains to be seen, but it certainly could lead to more unified care, better integrated data, and new opportunities to use analytics in improving population health. Stay tuned for more in 2018!
Ready for a test drive of our healthcare analytics software?
- Survey Says: Healthcare CIOs Don’t Fully Trust Their Data - November 8, 2018
- Microhospitals: How a New Healthcare Model Leverages Business Intelligence - September 25, 2018
- How New Database Technology Fuels Oil Company’s Analytics - September 20, 2018


