← Back to Healthcare stories
Navigating the New World of Quality-Based Reimbursement with Healthcare Analytics


Total Patient Revenue Model: Maryland’s Shift to Value-Based Care
Quality-Based Reimbursement: Western Maryland Health System transitioned from volume-based to value-based care, adapting to Maryland’s quality-based reimbursement model.
Total Patient Revenue Model: The TPR program aimed to achieve better quality, healthier patients, and reduced costs, driving the change from a fee-for-service model to a value-based approach.
Quality Indicators Tracking: Diver Platform enabled precise tracking of quality indicators, such as mortality and potentially preventable conditions, helping Western Maryland improve patient outcomes.
Accurate Readmissions Reporting: Dimensioal Insight solutions automated readmissions reporting, aligning with the Maryland Health Services Cost Review Commission (HSCRC) measures, resulting in accurate and timely readmission reports and frequent utilization reports.
Care Gap Closure: Dimensional Insight software helped identify discrepancies in patient information between systems, allowing Western Maryland to close the care gap and improve patient follow-up care.
Financial and Operational Benefits: The implementation of Dimensional Insight analytics solutions led to improved patient follow-up care, fewer discrepancies, fewer financial penalties, and a positive revenue swing.
Performance Improvement: Western Maryland reduced its readmission rate, moved from last place to first in quality-based reimbursement measures, and improved its performance and reimbursement significantly.
Background
Hospitals and health systems everywhere are trying to navigate the new world of healthcare. It seems like they must do everything at once — from improving patient care to reducing readmissions to cutting costs to gaining operational efficiencies. The reality is that these imperatives are not separate initiatives, but intertwined.
Federal initiatives such as the Affordable Care Act and the CMS Hospital Value-Based Purchasing (VBP) program provide incentives for improving healthcare quality and decreasing costs. As the incentives and penalties associated with these programs become more significant, clinging to a fee-for-service based model will become increasingly difficult for providers.
The State of Maryland is at the forefront of this change. It was the first state in the nation to be granted a waiver from Medicare rules, providing flexibility to implement its own quality-based program. The Maryland Health Services Cost Review Commission (HSCRC) sets hospital rates that apply to all payers, including Medicare and Medicaid, as well as self-insured patients. Starting in 2009, the HSCRC initiated payment adjustments to the hospitals’ rates according to their performance on a set of quality indicators that reflect care quality and patient outcomes. For a healthcare provider such as Western Maryland Health System, a 205-bed hospital in Cumberland, Md. that services a rural area across three states (West Virginia, Pennsylvania, and Maryland), this was a challenging proposition. In the first year under the quality-based Maryland reimbursement model, Western Maryland was ranked 46th out of 46 hospitals. It had to turn its system around by being prudent with its resources and gaining insights into changes that would help improve performance on the quality indicators that determine reimbursement.
This would be daunting for most hospitals — and it felt that way in the beginning for Western Maryland. However, the health system focused on implementing the right technology to enable greater insights focused on providing better patient outcomes. The goal was to provide the hospital with a one-two punch: identify ways to reduce costs while also improving the health of the population it serves.
Impetus for Change: Moving from Volume-based to Value-based Care
In 2010, 10 Maryland hospitals, including Western Maryland, volunteered to participate in a demonstration project called “Total Patient Revenue” (TPR). This was a test run for the global budget revenue methodology that all Maryland providers operate under today. The objectives of the TPR program were consistent with the goals of the Institute for Healthcare Improvement’s “Triple Aim”:
- Better quality
- Healthier patients
- Reduced costs
Under the new model, Western Maryland received fixed revenue for all inpatient and outpatient services provided in the hospital. As a result, this encouraged the hospital to provide the most appropriate care in the most appropriate setting.
| Fee-For-Service Model | Total Patient Revenue Model |
|---|---|
| Encourages caring for the ill and maximizing volumes. | Encourages wellness and cost-effective care. |
| Revenue varies based on volume. | Revenue is fixed and predetermined. |
| More admissions and outpatient volumes = more revenue. | More admissions and outpatient volumes = no more revenue. |
Under quality-based reimbursement, Western Maryland did not fare well in FY 2012, losing a total of $1.2 million in revenue due to its low performance.
Payment adjustments to hospital rates also are made according to quality measures that include: improving patient satisfaction and core measures, avoiding potentially preventable conditions, reducing hospital-acquired infections, and reducing readmissions. Hospitals are rewarded financially for achieving high quality.
By tackling care delivery on multiple fronts, Western Maryland was able to realize several benefits: improved patient follow-up care, fewer discrepancies, fewer financial penalties, and positive revenue swing.
Reality check: Western Maryland needed to improve quality indicators
Under quality-based reimbursement, Western Maryland did not fare well in FY 2012, losing a total of $1.2 million in revenue due to its low performance on core measures, patient satisfaction, and potentially preventable conditions.
In order to improve its bottom line, Western Maryland outlined several key initiatives, which included, in part:
- Shifting emphasis from volume to value
- Reducing admissions and readmissions
- Providing care in the most appropriate location
- Reducing variation in quality
- Reducing utilization rates in the emergency department, inpatient, observation, and ancillary
- Improving chronic care delivery
To achieve success, Western Maryland determined that it needed a business intelligence and analytics solution to better leverage its data. The health system wanted a solution that could be deployed quickly, would let users create their own dashboards and data views, and had the horsepower to aggregate data from multiple systems for better visibility. The solution would need to integrate data from Western Maryland’s data sources, which included: the MEDITECH electronic health records system, eClinicalWorks for ambulatory patient information, 3M for coding and care management, and Kronos for time and attendance.
The hospital looked at major business intelligence players, including SAP and QlikTech, as well as MEDITECH ecosystem vendors such as MediSolve. Ultimately, Western Maryland chose The Diver Platform (Diver) by Dimensional Insight.
“Diver enables us to get information into the right hands at the right time and do so more quickly and cost-effectively than could other business intelligence solutions we considered,” said William Byers, chief technology officer for Western Maryland Health System. “What also really impressed me about Dimensional Insight was that I was able to talk to its MEDITECH customers and verify the ease-of-use and results they were able to realize through the technology.”
As someone who would be interacting with Diver day-to-day, business intelligence analyst Colby Lutz appreciated the flexibility of the platform and the control it gave him over the organization’s data. “With other business intelligence tools, we would have to rely on the vendor to create a lot of the data views. Diver provides our facility with the flexibility to create a lot of these pieces myself so I can quickly get to the exact information I’m looking for.”
Once Western Maryland implemented Diver, it set forth on a series of specific projects aimed at using a data-driven approach to improving the quality of care it provides to patients. The results of this approach were realized quickly and dramatically.
The hospital looked at major business intelligence players, including SAP and QlikTech, as well as MEDITECH ecosystem vendors such as MediSolve. Ultimately, Western Maryland chose The Diver Platform (Diver) by Dimensional Insight.
“Diver enables us to get information into the right hands at the right time and do so more quickly and cost-effectively than could other business intelligence solutions we considered.”
First Order of Business: Tracking Quality Indicators
Under Maryland’s quality-based reimbursement program, mortality is one of the quality indicators that affects a hospital’s reimbursement. Once Western Maryland implemented Diver, it saw an immediate opportunity to use the platform to more precisely track mortality measures. The HSCRC measures mortality slightly differently than do other states. With Diver, Western Maryland was able to create formulas based on the HSCRC’s calculations, and then extract data on a continual basis to stay on top of its performance on the measure.
“Rather than using data that was a month or two old, we were able to stay ahead of how we were performing on this performance measure so we could implement changes immediately if we needed to,” said Tracey Davidson, quality manager at Western Maryland, who was one of those responsible for creating the mortality reports.
Next, Western Maryland began tracking potentially preventable conditions, another quality indicator that affects quality patient outcomes. By doing so, the health system was able to reduce the number of patients who acquired preventable conditions while in the hospital.
“We created an order set monitoring tool that would track compliance with patient order sets,” said Davidson. “It enabled us to quickly see which patients were not in compliance and look at their outcomes.”
For example, if a patient acquired sepsis while in the hospital, Western Maryland was able to quickly see what condition the patient was admitted for and whether the order set was in place allowing for further investigation when necessary. The health system could stratify the data to see which patients received care consistent with order sets and which did not. It also helped quantify the impact of compliance on outcomes. Using the data provided by this tool, Western Maryland was able to confirm that order sets were effective and needed to be followed. This information also helped facilitate the training process around order set compliance.
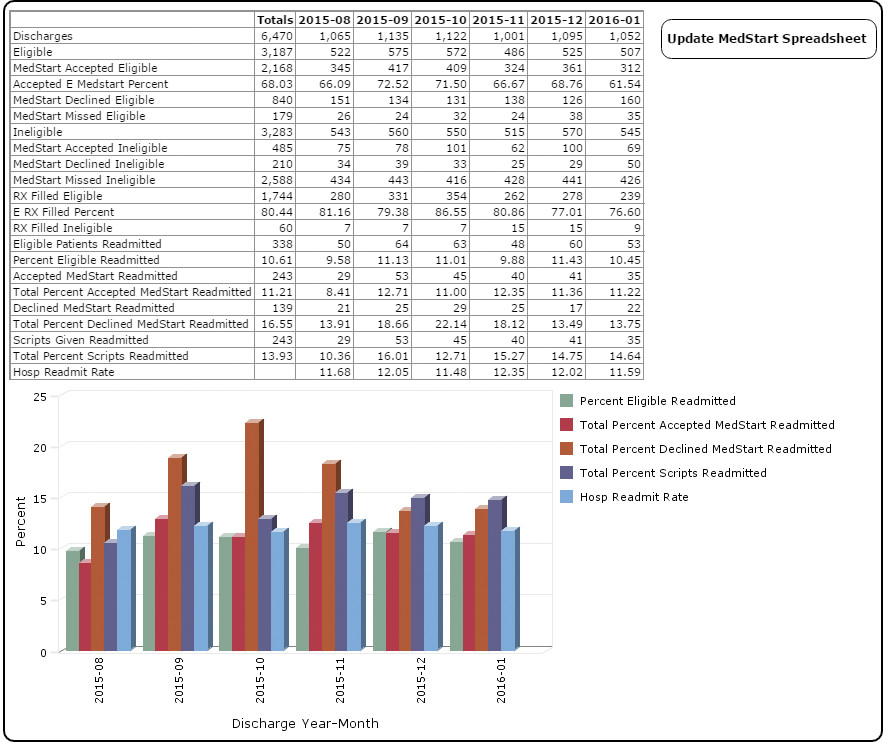
Next Order of Business: Getting an Accurate Read on Readmissions
Another quality indicator that Western Maryland needed to tackle was readmissions. Lowering 30-day readmissions is critical to improving patient outcomes under the Maryland model.
Prior to implementing Diver, the hospital relied on daily emails of MEDITECH census information to produce its readmission report. However, these readmission measures, which were based on the Centers for Medicare & Medicaid Services (CMS) definition, were calculated differently than the HSCRC version, resulting in slight discrepancies which could translate into financial penalties for Western Maryland.
To reconcile these differences, Western Maryland’s Director of Quality Initiatives would make corrections in an Excel spreadsheet — a time-consuming and inefficient process. To improve visibility and responsiveness, the hospital decided to automate readmissions reporting using Diver.
A team consisting of Western Maryland staff and Dimensional Insight consultants translated the HSCRC readmissions specifications into business rules and measures. The result was an accurate and timely daily readmission report plus a companion frequent utilization report that provides detailed patient information on those patients who were frequently readmitted. Together, these reports help medical teams and case managers to optimize patient care.
According to Lutz, “The increased level of data integrity made possible by Diver really helped us define what we were looking at, who needed to look at what, and how to best provide that information to specific users.”
The Pieces Come Together: Closing the Care Gap
With accurate readmissions reporting in place, Western Maryland staff next turned its attention to determining why patients were returning and how post-discharge follow-up care could be improved.
The CareLink coordination team, responsible for following up on high utilization patients after discharge, was one of several initiatives designed to implement process improvements. Diver captured all discharges from the MEDITECH EHR and 3M coding and care management system. These were then filtered to produce a call list of patients who met specific criteria for outreach. The report also enabled the CareLink team to determine whether patients declined certain services on discharge and whether they made it to follow-up appointments with primary care physicians.
This process brought to light discrepancies in discharge information between systems. For example, discharge dispositions were not matching on missed or added patients. How could the hospital provide follow-up care to patients who were in jeopardy of falling through the cracks if they couldn’t figure out where they were discharged to? Because Western Maryland reports to HSCRC using data from multiple systems, the hospital needed to ensure the integrity of its reporting. Using Diver, Western Maryland was able to create a discharge discrepancy report that compared the data in each system, helping to highlight and resolve inconsistencies. The hospital also implemented process changes so care managers could review mismatches during morning huddles and work with nursing staff to improve the accuracy of patient documentation and discharge orders.
Another change involved working with primary care providers (PCPs) who were having trouble seeing patients within five days of discharge. Western Maryland created a discharge clinic that patients could visit to ensure they understood their medications and were taking them appropriately, thereby helping to prevent lapses in care.
By tackling care delivery on multiple fronts, Western Maryland was able to realize several benefits:
- Improved patient follow-up care: Prior to the discharge discrepancy report, there were approximately 150 patient mismatches each month. Through the report, and system and process changes, there are now zero mismatches and the care gap has shrunk significantly.
- Fewer discrepancies: The number of discrepancies that HSCRC reported back to Western Maryland has decreased.
- Fewer financial penalties: Because there are fewer potentially preventable conditions, Western Maryland has avoided HSCRC penalties.
- Positive revenue swing: Western Maryland went from losing $1.2 million in quality-based reimbursement in FY 2012 to gaining $1.3 million in FY 2014.
Perhaps most importantly, Western Maryland’s patients have benefited from the improved insight, especially those high utilization patients. In 2011, there were 1,972 patients who accounted for $140 million in costs. By 2014, that number dropped to 1,300 patients with associated costs of $80 million.
Western Maryland went from losing $1.2 million in quality-based reimbursement in FY 2012 to gaining $1.3 million in FY 2014.
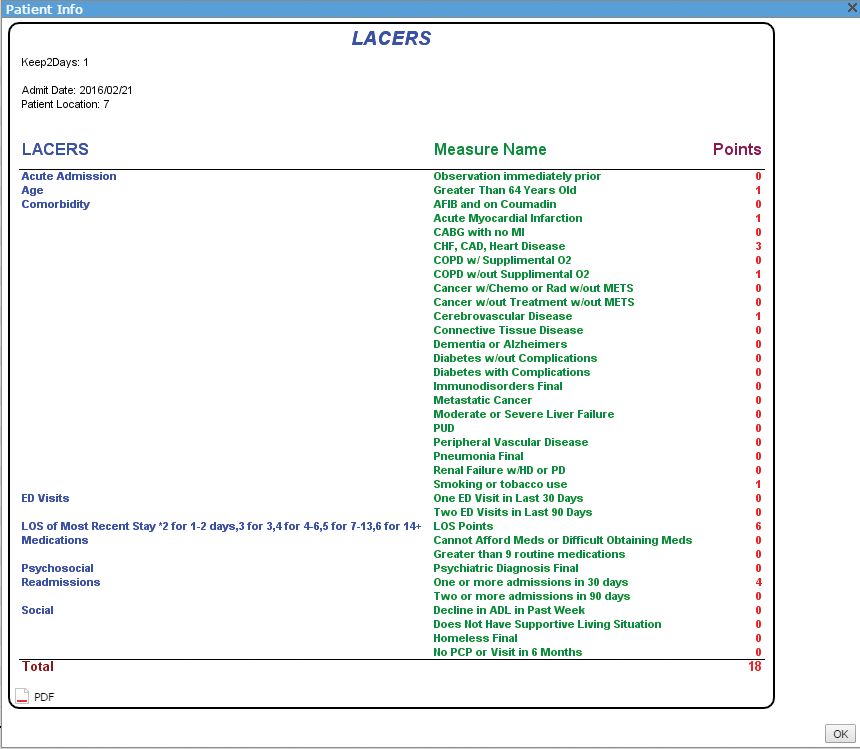
LACERS is run to see what patients are highest risk for readmission as well as used for extensive discharge planning based on the accumulation of points.
Catapulting to First: Driving Improvements to the Bottom Line
With its Diver-based internal reporting aligning reporting with HSCRC measures, Western Maryland was able to drive its readmission rate down to 11.72% — well below the Maryland average of 13.9%. It also went from last place out of 46 Maryland hospitals in terms of in quality-based reimbursement measures to first place in the state.
“When we first implemented Diver, we saw a real opportunity for business intelligence to drive change in our organization, and we ran with it,” said Lutz. “Diver enabled such deep insights that we saw an almost immediate and dramatic change in our performance and reimbursement.”
Looking Toward the Future: Continuing to Drive Change
The success of Diver with readmissions has also spurred interest in other Diver applications throughout the organization. For example, during Diver training, Western Maryland noticed that many patients were being admitted as “inpatient” to the Observation Unit, which is intended only for outpatients. In fact, the hospital is penalized for inpatient admissions to this unit. With Diver, Western Maryland was able to identify those patients and admit them correctly. Since this change, there have been zero inpatient admissions to the Observation Unit.
Western Maryland also uses Dimensional Insight’s Physician Performance Advisor application to measure the impact of physician practice patterns on health system performance. Physician Performance Advisor helps Western Maryland with its Ongoing Professional Practice Evaluation (OPPE), as required by the Joint Commission. But perhaps more significantly, it provides physicians with access to their own information so that they can both better understand how they are performing vs. their peers and identify opportunities to improve the care they provide to their patients.
“The benefits of Diver were immediately apparent to us in several areas of our organization,” said Byers. “Diver helps us spot trends and then dive down to the patient encounter level to enable us to see exactly what is going on inside our system so that we can make better, more informed decisions.”

Organization
Western Maryland Health System
Industry
Healthcare
Location
Cumberland, Maryland
Beds
205
Website
www.wmhs.com
Solution
Diver Platform
More Healthcare stories →